Abstract
In 2019, 142,670 Americans died of lung cancer— more than colorectal, breast and prostate cancer combined. Lung cancer remains the leading cause of cancer death. However, according to the American Lung Association (ALA), only 5.7 percent of the estimated 15 million eligible Americans at risk of developing lung cancer will undergo screening.
Lung cancer screening should be considered a process, rather than a single test. Following the initial LDCT scan, a yearly scan or additional tests may be recommended to assess the risk of malignancy of any incidental pulmonary nodules. Treatments are more effective, resulting in improved survival rates, with a robust screening program that combines early detection among high-risk persons (due to age or cigarette smoking history), timely patient tracking, and prompt follow-up care. Also, some healthcare organizations use manual tracking tools like Excel spreadsheets— mechanisms that can detract from the efficiency of their screening program and effectiveness of their clinical team. Growing evidence points to significant improvements in Lung Cancer Screening Programs (LCSP) with automated solutions, using advanced software.
The Thynk Health platform implements a systematic and automated patient outreach strategy, to get eligible high-risk persons in the door for screening. Further, Thynk Health’s platform uses natural language processing and advanced artificial intelligence to make lung cancer screening more powerful and scalable, ultimately empowering health care organizations to reduce mortality from lung cancer.
Introduction
Helical low-dose computed tomography (known as low-dose CT or LDCT) is the only recommended screening test for persons at high risk for lung cancer. Data from the National Lung Screening Trial, commissioned by the National Cancer Institute, showed that participants who received LDCT scans had a 15 to 20 percent lower risk of dying from lung cancer than those who received standard chest X-rays. LDCT can identify pulmonary nodules or other abnormalities in the lungs, which could indicate lung cancer at different stages.
Detecting a problem at an early stage, prior to symptom onset, may make it easier to treat. Additionally, patient smoking history or pack years requires review, tracking and follow up, including to encourage quitting cigarette smoking as a chief preventative measure, regardless of a negative test result. However, healthcare organizations are usually fragmented, as is their patient data, which is located in different repositories of structured and unstructured data.
To build and grow your Lung Cancer Screening Program (LCSP), partnership with a comprehensive management solution is most effective, in order to address the complexities of screening and pulmonary nodule management in an often fragmented healthcare environment. In 2019 MercyOne Des Moines Medical Center, a leading hospital in the US, partnered with Thynk Health, utilizing our complete lung cancer screening and incidental finding management solution to build an efficient and effective screening solution that increased lung cancer screenings among at-risk patients, automated data entry and patient tracking, while freeing up staff and physician resources to focus on patient care. They achieved a 76.2% increase in the number of new patients undergoing screening from 2018 to 2019. This experience is not unique to MercyOne Des Moines. We are vested in the success of every partner and our customer success rates, customer service, and software accuracy are unmatched in the industry.
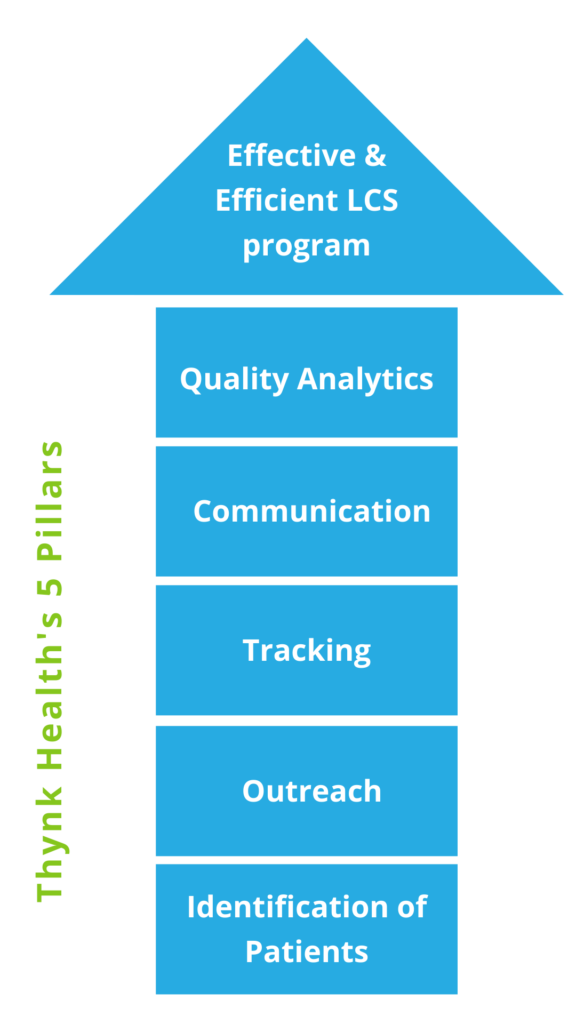
Thynk Health implements 5 basic pillars through our sophisticated software solution, designed to disrupt outdated and burdensome lung cancer screening processes. These 5 pillars are: identification of patients, outreach, tracking, communication and quality analytics.
Identification of Patients
The U.S. Preventive Services Task Force (USPSTF) recommends annual lung cancer screening, with LDCT, for a specific high-risk population who:
- Have a history of heavy smoking, that is, 20 pack years or more.
- Smoke currently, or quit within the past 15 years.
- Are between 50 and 80 years old.
This screening is currently covered by most insurance plans and Medicare.
The ‘Meaningful Use’ financial incentive program for electronic health record (EHR) adoption in the U.S., requiring healthcare providers to capture a patient’s smoking status electronically, has helped to standardize data collection of this and other information. However, with a relatively short history of 10 years, ‘Meaningful Use’ came into full effect gradually, allowing data quality issues to persist. This, compounded by the challenge of fragmentation within healthcare organizations, with patient data often located in different repositories, demands a thorough solution to prevent at-risk individuals from falling through the cracks. Thynk Health’s complete cancer screening and incidental findings management solution identifies at-risk patients using advanced natural language processing to extract critical information from unstructured data. Data from multiple sources including: DICOM data, clinical notes and OP clinics affiliated with your healthcare organization can be integrated and normalized. Examining medical history and demographics, Thynk Health’s LDCT Module tracks information around nodule stability and flags patients at a higher risk of lung cancer, to notify care teams.
Outreach
Evidence shows that timely screening and prompt patient follow-up saves lives, as stakeholders are empowered with actionable information. An effective LCS program should therefore invest in a systematic patient and provider outreach strategy. Postcards, letters, and certified mail can be automatically mailed to eligible, high-risk patients that have not sought screening, or lack updated EHR records; scorecards can be sent to providers to help them understand where they may be falling short in comparison with their cohorts in ordering screening for certain patients; and general information on the progress of your health organization’s screening program can be disseminated. Thynk Health offers an automated solution to patient and provider outreach that is fully customizable, depending on the policies of your healthcare organization. As manual processes of patient outreach are automated, clinical teams can focus on improving patient care and ultimately benefiting patient outcomes.
Tracking
More than 1.5 million Americans will have a pulmonary nodule identified every year. Only 29 percent will receive appropriate follow-up care.
When building a lung cancer screening program, your healthcare organization must prepare not only for screening and reporting results, but for tracking patients who may miss screening appointments, require annual screenings, and require follow-ups due to incidental findings. Manual techniques are not practical or an efficient use of your care team’s abilities. An automated approach for tracking patients through a long, and often complicated, treatment journey is necessary to ensure each patient receives the necessary care. Further, Thynk Health’s solution automatically submits patient data to the American College of Radiology (ACR).
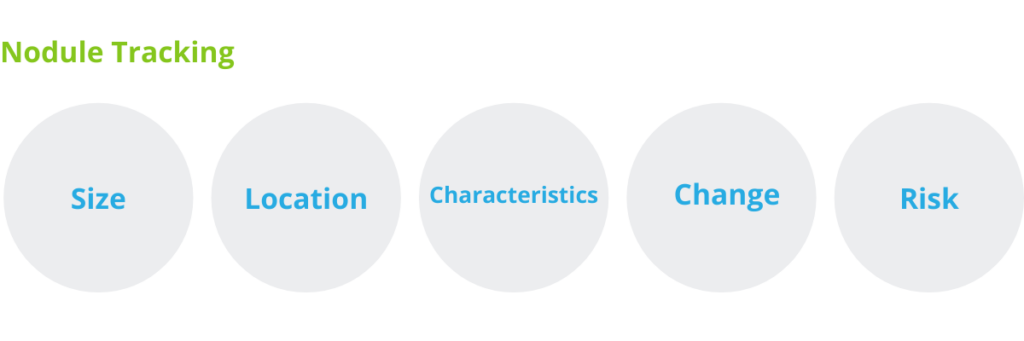
To ensure patients are properly informed and cared for, incidentally identified pulmonary nodules should be automatically labeled and tracked for appropriate follow up. This also helps to minimize risks associated with malpractice due to miscommunication or inaction regarding incidental findings. Thynk Health’s Nodule Nav solution processes radiology reports to extract the number of nodules, nodule size, location, and nodule characteristics. This empowers partner healthcare organizations to automatically track nodule changes within each appointment, flag nodules for follow-up, and recommend next steps.
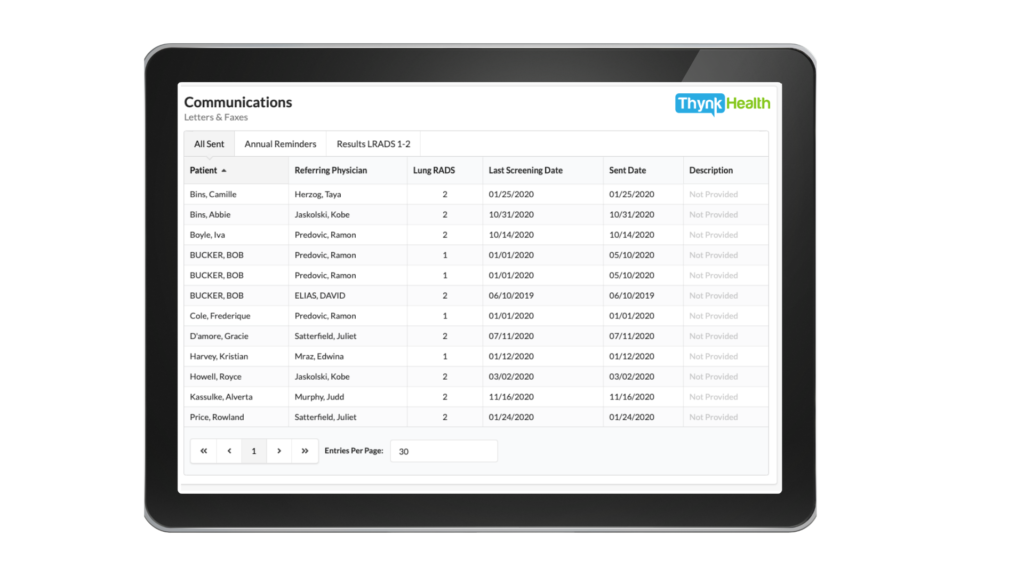
Communication
Automating communication frees clinical teams to focus on patient care, rather than correspondence management. Thynk Health eliminates manual mailing tasks often left to nurse navigators by automatically sending reminders and results letters to patients and providers. Thynk Health is the only solution that does not require the navigator to download letters, print, and manually stuff and send envelopes. Additionally, Thynk Health’s lung module automatically shares important information with primary care physicians, like the number of their patients currently eligible for lung cancer screening and the number of screenings ordered.
Quality Analytics
A trusted analytics partner will augment a data-driven culture within a lung cancer screening program. Regular analytics reports, intuitive and efficient dashboards, as well as routine calls from your analytics partner provide actionable information that benefits the growth of the LCS program. Thynk Health’s solution helps healthcare organizations focus on, and rectify any deviations to what is considered standard and quality practice. Additionally, Thynk Health operational analytics help healthcare organizations observe volume shifts or changes to ensure recovery of downstream revenue, as well as execute effective targeting of all their eligible population, to get patients in the door.
Conclusion
“Forward-thinking organizations have already started to view lung cancer screening as an important population health initiative.” – Joey Bargo, Chief Clinical Informaticist at Thynk Health.
To drastically lower the mortality of the leading cause of cancer death in the US—lung cancer, screening programs must be built and bolstered to be more accessible, scalable, and powerful. At Thynk Health, we are confident that our state-of-the-art technology will fit perfectly with fast-growing and innovative healthcare organizations who share our goal of saving lives. With more than 100 years of healthcare management experience at Thynk Health, we were able to provide unique insights and guidance throughout the process of building and growing your lung cancer screening program, to achieve the best possible results.
Learn how Thynk Health can your build and grow your lung cancer screening program.
1-855-633-6963 | thynkhealth.com
Resources
- https://www.cdc.gov/cancer/ncccp/pdf/LungCancerScreeningPrograms.pdf
- https://lcfamerica.org/lung-cancer-info/lung-cancer-facts/#1548796105763-eb87ec3a-6bfc
- https://www.cancer.org/content/dam/cancer-org/research/cancer-facts-and-statistics/annual-cancer-facts-and-figures/2019/estimated-deaths-for-the-four-major-cancers-by-sex-and-age-group-2019.pdf
- “Age, comorbidity, life expectancy, and pulmonary nodule follow-up in older veterans”, US National Library of Medicine National Institutes of Healthhttps://www.ncbi.nlm.nih.gov/pmc/articles/PMC6059441/
- “Not All Lung Nodules are Cancerous But Follow-up Care is Important”, Holly Stilz, PA., clinic coordinator at the UK HealthCare Lung Nodule Clinic https://uknow.uky.edu/uk-healthcare/not-all-lung-nodules-are-cancerous-follow-care-important
- https://go2foundation.org/
- https://go2foundation.org/risk-early-detection/risk-factors/
- https://www.cancer.gov/types/lung/patient/lung-screening-pdq
- https://www.ahra.org/AM/Downloads/PatientsFirstProgram/Articles/RM376_p42-46_Features.pdf
- https://www.appliedradiology.com/articles/a-five-step-strategy-for-building-an-ldct-lung-cancer-screening-program
- https://www.cancer.gov/types/lung/research/nlst
- https://www.ncbi.nlm.nih.gov/pmc/articles/PMC5977725/
- https://journal.chestnet.org/article/S0012-3692(21)00223-3/fulltext